|
Everyone experiences stomach pain at least once. The good thing about stomach pain is that it disappears on its own and usually requires no further medical intervention. On the other hand, severe cases of stomach ache pertaining to infections and disorders require immediate medical assistance. So, what are the causes of upper stomach pain? It can be anything from a ruptured spleen to excess gas in the intestine. Knowing the location, trigger, and kind of pain will help doctors accurately identify the cause of upper stomach pain. Understanding the Upper AbdomenStomach pain is usually caused by gas, indigestion, and excessive stomach acid. Various home remedies can be applied to alleviate discomfort in this area. On the other hand, this common discomfort can also be attributed to reasons not concerning the stomach. The upper stomach, or more accurately the upper abdomen, houses numerous organs that could easily be the real reason for stomach pain. These organs include:
These vital organs can be subjected to infections, inflammation, and other disorders that could result to pain. Understanding the different parts of the upper abdomen makes it easier to diagnose the real cause behind stomach pain. Causes of Upper Abdominal PainMuscle PainMuscle pain is one of the most common sources of abdominal pain. Also known as muscle soreness, this type of pain is caused by strenuous or sudden activities that may result in a sore or pulled muscle. Stiffness, cramps, weakness, and limited mobility are signs of muscle soreness. Pain heals naturally in a matter of days or weeks, depending on the severity of the trauma. DyspepsiaDyspepsia, more commonly known as indigestion, is characterized as a burning sensation in the upper stomach. This pain can radiate to the chest, typically described as a lingering “fullness”. Dyspepsia is triggered by highly acidic and spicy foods, as well as stomach ulcer. Overeating is also a known cause of acute indigestion. Dyspepsia is a common condition and isn’t considered a disease. On the other hand, chronic indigestion is typically caused by other gastrointestinal conditions such as infection, liver diseases, peptic ulcer, gastric cancer, and inflammatory bowel disease, to name a few. GasPain that is accompanied by burping, passing gas, and bloating are all common signs of excess gas in the intestine. Gassiness can also result to pain that feels like something is moving in the stomach. Episodes are sporadic and heal over time. However, persistent gassiness can point to more serious problems relating to a virus or infection in the digestive tract. In this case, immediate medical intervention is recommended. GallstonesGallstones are one of the most common causes of upper stomach pain for patients thirty years old and above. There are two types of gallstones: cholesterol stones caused by high levels of cholesterol in the bile; and pigment stones caused by excessive levels of bilirubin in the bile. Gallstones may pass on their own, but blockage caused by the build-up may result in strong intense pain in the upper right part of the abdomen. Fatigue, exhaustion, vomiting, and jaundice are telling signs of gallstone blockage. In minor cases, doctors will recommend medication that will help break down the gallstones. Gallbladder removal may be prescribed to completely alleviate a patient’s pain and discomfort. Peptic UlcerStomach acids and bacterial infection can result in the development of sores along the stomach lining, known as peptic ulcer. There are three known types of peptic ulcers:
Pain from peptic ulcer is characterized as pain that travels from the chest to the bottom of the abdomen. Pain can also be caused by hyperactive stomach acids, which is why patients suffering from peptic ulcer are recommended to always have a full stomach. Changes in appetite, indigestion, and vomiting are common signs of peptic ulcer. Spleen ProblemsThe two most common spleen problems are splenomegaly and a ruptured spleen. Splenomegaly, known as an enlarged spleen, is caused by liver diseases and infections. On the other hand, a ruptured spleen is caused by trauma on the abdomen, usually through sports or a car accident. An enlarged spleen can press on the stomach, resulting in a “heavy” pain in the abdomen that often radiates through the shoulders. Discomfort on the ribs is also characteristic of splenomegaly. Abdominal pain is not a common symptom of a ruptured spleen and only occurs in rare cases. When experienced, alongside pain in the left shoulder, patients are recommended to immediately seek medical help. GERDGastroesophageal reflux disease (GERD) is a chronic condition caused by a faulty lower esophageal sphincter (LES). The LES serves as a valve between the esophagus and stomach. When it relaxes, stomach juices are regurgitated up the esophagus, creating a burning sensation accompanied by a sour or bitter taste. Pain from GERD is described as a sharp, acidic pain that radiates from the stomach to the esophagus. Bad breath is a common symptom of GERD. Other symptoms include chest pain and heartburn. GastritisExcessive alcohol use and the presence of bacteria are leading causes of an inflamed stomach lining, leading to gastritis. Other causes include the body’s natural interaction with medication, long periods of stress, and inflammatory problems concerning the immune system. Chronic gastritis has been characterized into three distinct types:
Pain that can be described as a gnawing sensation, one that typically worsens after meals or at night, is a telling sign of gastritis. Nausea, loss of appetite, and bloating are other symptoms of gastritis. Pain is usually located in the upper left area of the stomach or the center of the abdomen. PancreatitisPain from pancreatitis is often situated in the middle or upper left side of the abdomen, and is described by patients as a pain that radiates towards the back. Eating excessive amounts of food, especially foods with high-fat content, and alcohol abuse are known triggers of pancreatitis. Excessive alcohol consumption and the presence of gallstones cause 80% of pancreatitis cases. Pancreatitis occurs when digestive juices are activated in the pancreas. The small intestine is responsible for breaking down fat with the use of digestive enzymes. However, these enzymes can be activated while in the pancreas, leading to inflammation and possibly infection. HepatitisHepatitis describes five types of liver inflammation caused by different viruses. Hepatitis is a viral disease that can be transmitted through blood transmission, sexual contact, and hereditation. The five different types of hepatitis are:
Pain caused by hepatitis is often described as a stretching, likely associated with the expanding of the liver due to inflammation. This discomfort is more characteristic of hepatitis C and is rarely experienced in other types of hepatitis. Upper Stomach Pain: When Is It Serious?Stomach pain passes on its own in a matter of days. However, persistent pain or additional symptoms may signal something serious and urgent. Seek immediate medical attention if the patient is experiencing the following:
Treat Stomach Pain For GoodLearn more about the various causes of abdominal pain in general by getting in touch with us. At the Gastro Center in New Jersey, we are always ready to help patients learn more about their concerns. Book an appointment today and let us diagnose and treat your pain. The post Why Do I Have a Stabbing Pain In My Upper Stomach? appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/stabbing-pain-in-upper-stomach/
0 Comments
Breakfast has always been hailed as the most important meal of the day. Turns out this old adage is nothing short of true, especially for acid reflux sufferers. Filling up the stomach with good food can prevent acid attacks throughout the day and alleviate symptoms of acid reflux. What kind of breakfast foods are suitable for people with acid reflux? The idea is to eat alkaline foods that won’t contribute to or trigger reflux symptoms. This includes oatmeals, select fruits and vegetables, as well as lean protein. Distinguishing good and bad food for acid reflux is the key ingredient to starting your day right. Signs You Have Acid RefluxBurping? Constipation? Stomach cramps? You might think you’re just experiencing morning hunger pangs when you’re actually experiencing acid reflux. Acid reflux is a common disorder that happens when a muscle called the lower esophageal sphincter (LES) fails to seal in stomach juices. When the LES relaxes or malfunctions, stomach acid can move back up the esophagus, causing burning in the throat accompanied by a sour taste. Other signs of acid reflux include:
How Can Food Trigger Acid Reflux?Although there is no clear proof that certain food groups can cause acid reflux, it is known that specific foods can trigger or aggravate existing symptoms. Food can be used to minimize the acidity of stomach contents by adjusting the diet accordingly. Some foods can even cause the LES to relax, which could worsen the regurgitation of stomach acids. 6 Breakfast No-Nos: What to Avoid1. Foods with high fat contentStudies show that people who consume food with high levels of cholesterol and saturated fat are likelier to experience acid reflux symptoms. Fatty foods take longer to break down than their healthier counterparts. The stomach is forced to produce more acid in order to properly digest these foods, leading to heartburn. Foods considered high in fat include anything deep fried. Ham, bacon, french fries, onion rings, and just about anything dripping with oil are clear examples of foods to avoid when experiencing acid reflux. 2. CaffeineCaffeine, both in coffee and energy drinks, should be avoided by acid reflux sufferers. Caffeine is known to relax the LES, causing acid reflux, but this varies depending on a person’s digestive tract. High amounts of caffeine also translate to higher acidity, which can further aggravate an already irritated digestive system. However, it’s still possible to enjoy a cup of coffee in the morning without inducing heartburn. For starters, you could look into coffee options that have a lower caffeine content such as decaffeinated coffee and a latte. Opting for low-caffeine drink alternatives such as tea is also a viable breakfast option. Note that some teas are actually acidic in nature. Mint-based may exacerbate reflux symptoms. 3. Spicy foodsSpicy foods are included on the National Institute of Diabetes and Digestive and Kidney Diseases list of foods that worsen acid reflux. Spicy foods are known to act as irritants that may decrease LES functionality, leading to heartburn. These also encourage the production of stomach acid, which doesn’t help an already passive LES. 4. ChocolateChocolate contains certain components that irritate the stomach such as caffeine, theobromine, and methylxanthine. Its primary ingredient, cocoa powder, is also acidic in nature. On the other hand, some chocolates may be more accommodating to a sensitive stomach; dark chocolate has a lower acidity level than full-fat chocolate. 5. Acidic fruits, vegetables, and condimentsWhile fruits and vegetables are generally recommended to any diet, acid reflux sufferers should be wary about consuming too much of certain foods. These include oranges, grapefruits, lemons, limes, tomatoes, pineapple, and any other food that is high in acidity. By-products of these fruits and vegetables, including lemoned, pure fruit juices, and salsa, should be consumed in moderation or avoided altogether. The Most Important Meal Of The DayThe act of eating breakfast alone is known to help manage chronic acid reflux. By eating something in the morning, acid reflux sufferers give their empty stomachs something to digest. Instead of travelling up the esophagus, the acids can work on healthy breakfast food, reducing feelings of constipation and stomach cramps. Eating early in the morning can also calm the stomach and prevent symptoms throughout the day. On the other hand, skipping breakfast is known to both induce and worsen acid reflux symptoms. Top Breakfast Foods For Fighting Acid RefluxPlanning meals may feel more challenging when eating with acid reflux sufferers. However, there are still food options available for people with even the most sensitive of stomachs: Alkaline Fruits and VegetablesApples, bananas, coconuts, apricots, avocados, pears, and blueberries are examples of alkaline fruits. Swap out acidic fruits for these and add them as toppers for your cereal, oatmeal, or pancake. Potato, squash, and zucchini are among the breakfast-friendly, alkaline vegetables. Mash and bake these vegetables together to make healthy tater tots. OatmealOatmeal is an amazing powerfood with little to no acidic content. Oatmeal keeps you fuller for longer, is easy to digest, and is incredibly nutritious. Mix in a cup of almond milk or half a cup of skim milk for added flavor. Add in low-acid fruits such as apples and bananas to make your oatmeal a little more special. GingerGinger boasts of anti-inflammatory properties that can improve food digestion and prevent post-meal acid reflux. Swap out your morning coffee and tea for steeped ginger tea. Top off with a spoon of honey. Leafy GreensVegetables such as spinach, lettuce, and kale can be transformed into a healthy breakfast meal. Toss a boiled egg and some chicken bits with some shredded lettuce to make a delicious breakfast salad. Spinach and kale can be chopped, along with mushrooms and peas, for a yummy morning omelette. Leafy greens are low-acid, high-volume foods that will help neutralize acid in the stomach. Chicken and turkeyLean protein such as chicken and turkey make great breakfast meals. Use ground pork or turkey to make breakfast meatballs, nuggets, and strips to enjoy every morning. To keep lean meat safe for acid reflux sufferers, consider baking them in an oven instead of tossing them in a frying pan. Almond or Soy MilkCereal, oatmeal, and breakfast muffins don’t have to be boring. Adding a splash of almond milk or soy milk can take breakfast to a whole new level. Take note that not all nut-based milk have the same pH. Cashew milk, for instance, is considered an acid-forming food, and may induce acid reflux at breakfast. Breakfast Ideas For Acid Reflux
Breakfast Recipes for Acid RefluxDairy-Free PancakeIngredients: 1 cup of all-purpose flour 2 teaspoons baking powder 1 cup unsweetened almond milk 1 large egg 1 large egg yolk 1 ½ teaspoons canola oil 2 tablespoons sugar 1 can spray cooking oil Instructions: 1. Add wet ingredients and dry ingredients alternately. Keep mixing until all contents are incorporated 2. Spray pan with oil then pour mix 3. Cook until soft brown or no bubbles are showing OmeletteIngredients: 2 large eggs Minced mushrooms (or any other alkaline vegetable) Diced spinach (or any other leafy green) Salt and pepper to taste Instructions 1. Whisk both eggs onto a bowl, then add vegetables. You may also choose to brown the vegetables for 5 minutes before adding them to the egg mixture 2. Heat oil in a pan 3. Pour mix and wait for the omelette to form No-Bake Faux Banana BreadIngredients: 4 large ripe bananas 1 large egg 2 tsp honey (optional) 1 can spray oil 1 tbsp cinnamon powder Instructions: 1. Mash ripe bananas onto a bowl, then add egg. Whisk together. Add cinnamon powder and honey 2. Spray pan with oil 3. Pour mix onto the pan and wait for it to form Tater TotsIngredients: ¼ cup carrots ¼ cup sweet potato ¼ squash 1 tablespoon flour Salt and pepper to taste 1. Preheat oven to 450 degrees Fahrenheit 2. Peel and boil carrots, sweet potato, and squash. When soft, drain, and shred 3. Mix vegetables with flour, salt, and pepper 4. Form into small balls and bake for 20 minutes or until golden brown Making Breakfast Easy: Tips For Acid Reflux Sufferers1. Keep A Food Diary: Not all foods create the same reactions in people. Experiment with certain foods and see which ones aggravate your symptoms. Knowing how certain breakfast foods interact with your stomach makes it easier to plan meals in the future. 2. Don’t Lie Down Immediately After Eating: Go for a walk or sit up and use the computer. Lying down can cause indigestion, which can make acid reflux worse. 3. Take Antacids. Over-the-counter antacids are available to help keep acid attacks at bay. Take a recommended dose after eating breakfast to prevent stomach contents from travelling up the esophagus. 4. Eat Less, More Frequently. Overeating is a trigger of acid reflux. Eating less more frequently can prevent a sensitive digestive system from producing too much stomach acid at a time. Eat small snacks in-between meals or divide a big breakfast into two smaller servings/ 5. Look For Alternatives. Are there certain breakfast staples you can’t do without? It’s still possible to enjoy them by identifying key ingredients that make the food acidic. Craving for french toast? Swap full-fat milk with skim milk or soy milk. Skip the butter and use coconut oil instead. Eating the right kind of breakfast is just one way patients can keep acid reflux under control. Get in touch with us to learn more about acid reflux, both chronic and short-term, and how to deal with these accordingly. The post What Is the Best Breakfast for Acid Reflux Sufferers? appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/what-is-the-best-breakfast-for-acid-reflux-sufferers/ GERD and bad breath usually go hand-in-hand, but that doesn’t mean you have to live with bad breath forever. In this article, we discuss the cause of acid reflux, as well as some immediate remedies you can apply right now to improve your breath. So, how do you treat bad breath from acid reflux? Medicinal intervention is usually applied to more advanced cases, but making lifestyle changes are great for getting long-term results. Quitting smoking, limiting alcohol and caffeine consumption, and taking antacids are all great ways to alleviate acid reflux and prevent bad breath. What Is Acid Reflux Acid reflux, also known as heartburn, is a common condition characterized by pain in the lower chest. This usually happens when stomach acids bubble up to the esophagus, the tube moving food from the mouth down to the stomach. A muscle called the gastroesophageal sphincter is responsible for keeping stomach acid right where it belongs. However, certain triggers can cause the “valve” to malfunction, and the acid is brought back up to the esophagus. Other contents including bile and undigested food particles can also make their way to the esophagus. Although common, acid reflux can develop into a chronic condition. Persistent acid reflux symptoms that manifest more than twice a week will be characterized as GERD or gastroesophageal reflux disease. At this point, physicians may recommend medical intervention to manage the disease. Can acid reflux give you bad breath? Aside from heartburn, the most common complaint of patients experiencing acid reflux is bad breath. Stomach contents may regurgitate back to the esophagus, including any stomach acids, bile, and undigested food that will linger in your esophagus and creep up your pharynx, causing bad breath. Can acid reflux cause you to smell your own bad breath? Acids attaching to the walls of your esophagus can be smelled by other people. This is because gas particles can also attach to the tongue, which can aggravate the bad smell. Patients with acid reflux often report burping, which can also intensify the smell of the stomach acid. On the other hand, acid reflux breath may also be smelled by the patient. In some cases, patients report smelling their own breath even without opening their mouth. Bile wafts from the stomach up to the nose, which produces a pungent, often acidic smell. What does acid reflux breath smell like? Acid reflux on its own smells like bile. Anything sulfuric, pungent, strong, and acidic can be characterized as acid reflux smell. Patients also report different smells based on the medicine they are taking to manage GERD. Any sort of smell present in the mouth can be symptomatic of ulcers and other gastrointestinal problems. We recommend getting checked by a physician to rule out acid reflux and other possible diseases. Signs Your Bad Breath Is Caused By Acid Reflux Bad breath is typically managed by flossing, brushing the teeth, and using mouthwash. However, more persistent cases of bad breath could point to problems that don’t have anything to do with the mouth. Here are some signs that bad breath is being caused by acid reflux: 1. It’s related to food. When bad breath seems to follow any eating pattern, it may be because of gastrointestinal problems. Whether it’s eating too much or too little, eating spicy or sour food, the point is that the bad breath is triggered by a feeding pattern. When you observe that the bad breath comes after drinking coffee, it could be that the acid in the coffee is triggering stomach acids, leading to bad reflux. Test out your breath after eating certain foods and see if any feeding habits trigger bad breath. 2. It coincides with other digestive symptoms. Constipation, bloating, burping, and pain can all be signs of acid reflux. This is especially true when digestive symptoms come right after a feeding pattern. After drinking coffee, do you experience cramps in your lower abdomen? Do you start burping and experience a strong metallic taste in your mouth? Paying attention to your body’s physical reactions to food is an effective way of ruling out the cause of bad breath. 3. Your breath smells sour or acidic. Bile is commonly described as sourness accompanied by a burning sensation. Stomach acid backflow into the esophagus usually comes in the form of bile, which is a distinct sign of acid reflux and indigestion. 4. It gets worse with caffeine, alcohol, and tobacco use. Acid reflux is caused by the gastroesophageal sphincter weakening, leading to regurgitation of stomach contents back to the esophagus. Ingredients in caffeinated and alcoholic products are known to weaken the gastroesophageal sphincter. Other foods such as chocolate, foods high in fat and acid, as well as mint, onions, and garlic may produce the same reaction. 5. You feel discomfort in your throat. Acid backflow is usually accompanied with a strong acidic sensation in the throat, precisely because the acid is not meant to occur outside the stomach. If your throat feels scratchy, itchy, or tingly after burping, these are clear signs of acid reflux. A burning sensation in the throat accompanied by bad smell is a telling sign you have stomach problems. 6. Your tonsils are affected. Some patients may instinctively visit their dentist for a consultation after discovering that they have bad breath. Dentists can provide a preliminary diagnosis by ruling out the cause of bad breath. Inflammation around the throat, together with acid erosion on the teeth, are signs to watch out for. Your dentist may recommend a visit to a physician after the dental exam once signs of irritation are found. The Causes of Bad Breath From Acid Reflux Acid reflux itself isn’t the reason behind bad breath. There are two ways this situation could aggravate the smelly symptoms, and cause longer episodes of foul oral breath: 1. Tooth Decay: The stomach may be exposed to these strong acids, but it is also lined with a protective barrier that keeps the acid from “burning” the stomach. However, other parts of the body don’t have this lining and will be susceptible to acid damage, given prolonged exposure. Over time, acid wafting up through the esophagus and to the mouth can cause teeth to slowly erode and rot. The build up of decaying matter around the teeth could contribute to the bad smell, especially after the teeth rots. Maintain proper oral hygiene to prevent plaque and bacteria accumulation on and between your teeth. 2. Bacteria In Mouth and Throat: The esophagus is designed to be a highway for the food from the mouth to the stomach. With acid reflux, there is a backward flow or particles that are not meant to stay in the esophagus. When left untreated, bacteria can grow on the walls of the esophagus, leading to bad breath. Irritation, itchiness, and a tingling sensation are signs of bacteria presence in the throat. Home Remedies For Acid Reflux Breath
Treating Bad Breath From Acid Reflux Getting Rid Of Bad Breath From Acid Reflux One definitive way to treat bad breath is to treat the cause of acid reflux. Triggers can be anything from simple lifestyle choices to treatable gastrointestinal problems. Common causes include: Lifestyle
Medical
Treating Acid Reflux: When Will It Go Away? Acid reflux usually goes away on its own. On the other hand, those with chronic acid reflux or GERD may be prescribed with medication to help with acid reflux. Not all GERD medication are compatible with one patient, so it may take a while to find the right treatment. Bad breath can go away in as little as a week up to three weeks, depending on your treatment plan. Quick Fixes The best way to get rid of bad breath caused by acid reflux is to treat acid reflux itself. On the other hand, knowing some quick fixes can help you get through an entire day without having to worry about acid reflux breath:
Do you think your bad breath is a sign of a stomach problem? Book a consultation with us today to get a proper diagnosis on your stomach health. The post Acid Reflux and Bad Breath appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/acid-reflux-and-bad-breath/ When you feel like the contents of your stomach can make an appearance at any moment, the last thing you want to do is exercise. But just because you have acid reflux doesn’t mean you have to skip the gym and stay at home. So, does working out actually make acid reflux worse? This all depends on the kind of exercise you do and the precautions you take before working out. Low-impact exercises such as yoga and swimming won’t make your acid reflux worse. Adopting better feeding habits before going to the gym can also save you the trouble of burping bile throughout the day. Acid reflux and working out don’t always have to go hand in hand. There are plenty of things you can do to improve your symptoms while staying in shape. Understanding Acid RefluxAcid reflux refers to the “backflow” movement of gastrointestinal contents from the stomach up to the esophagus. A small muscle called the lower esophageal sphincter (LES) serves as a barrier between the stomach and the esophagus. This part of the stomach serves as a one-way valve, ensuring that no acid ever goes back up to the esophagus. But sometimes, certain triggers can weaken the LES, causing stomach contents to be regurgitated upwards. This results in acidic, pungent bile wafting onto the throat, typically accompanied by a burning sensation. The Relation of Exercise With Acid RefluxCan exercise induce acid reflux?Getting a good workout is a crucial part of any healthy lifestyle, but sometimes too much working out can be the very cause of heartburn. Exercise-induced heartburn is a common occurrence that can happen to anyone, at any age. Working out triggers acid reflux under certain conditions. These include:
Can exercise make existing acid reflux worse?Physical activity alone won’t make acid reflux worse, but certain movements will certainly do the trick. As explained by Dr. Eitan Rubinstein, an affiliated gastroenterologist with the Harvard Medical School, “Anytime you do anything strenuous, your stomach can tighten up, making contents flow upward, so anything can give you reflux if you strain yourself hard enough.” She also explains how rapid breathing, something that is unavoidable in aerobic exercises, can cause the lungs to expand which “can draw reflux material into your esophagus”. Specific activities are more prone to disturbing the stomach than others. She identifies any activity that involves bobbing up and down to be the main culprits for aggravating pre-existing acid reflux (source).
List of Exercises That Aggravate Acid RefluxNot all physical activities are created equally, with some more harmful to your stomach than others. For example, a study suggests that weightlifters had higher instances of acid reflux during an 80-minute rest period than marathoners and cyclists (source). Certain exercises are likelier to put pressure on the stomach, impede blood flow around the gastrointestinal area, both of which are considered triggers for acid reflux. Introducing huge amounts of air to the esophagus through gulping or breathing may also affect the LES. Some athletic mechanics involving bending the waist and hanging upside down may also cause heartburn. These exercises include:
Tips on Managing Acid Reflux Before Exercise
Approved Exercises for Patients With Acid Reflux
YogaYoga promotes flexibility, stability, and strength, without putting a strain on the abdomen. Although this low-impact exercise is generally considered one of the best ways to stay active for patients with acid reflux, be wary of inverted poses. Poses like downward dog and handstands may irritate the stomach and push the acid forward. Instead, stick to poses that don’t defy gravity. SwimmingSwimming is the ultimate aerobic exercise for patients suffering from acid reflux. Muscle strength and cardiovascular endurance are still tested, without putting unnecessary strain on your gastrointestinal area. WalkingSwap out running and jogging for something a little more low-impact. In a recent study, going on a 10-minute walk every week can reduce the chances of early death (source). Walking is a great way to stay active without stressing the digestive tract. The best part is that you can do this exercise outside the gym and make it a part of your lifestyle. FAQ – Acid Reflux and Working OutIs it safe to exercise when I have acid reflux? You’ll be fine as long as you stick to exercises that are approved for patients with acid reflux. In fact, some doctors even suggest gradually moving towards medium- to -high-intensity exercises, for as long as the body doesn’t exhibit aversion to these types of exercises. We recommend getting a physical trainer to learn more about exercises suitable for your situation. Is there a way to prevent acid reflux altogether? Acid reflux can be caused by medical complications such as a hiatal hernia or poor lifestyle choices. Staying away from working out won’t fix acid reflux, although it may temporarily alleviate symptoms. The best way to cure acid reflux is to get to the root of the matter and implement any dietary, lifestyle, or medical changes necessary. Choose Wellness, Choose PleasantdaleUnderstanding what’s causing your acid reflux is the only way you can prevent the symptoms from appearing. Book an appointment with us to learn more about your gastrointestinal health. Let’s get in better shape, together. The post Does Working Out Make Acid Reflux Worse? appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/does-working-out-make-acid-reflux-worse/ The colonoscopy is the golden standard for catching polyps and preventing colon cancer altogether. So if it’s so effective, why are patients so averse to undergoing a colonoscopy, even if it means saving their lives? There’s only one reason: the dreaded prep drink. Colon preps are infamous for being extremely uncomfortable and arduous. In the article below, we explain everything you need to know about these drinks, and how you can manage through yours to ensure you have comfortable colon prep. Breaking Down Colonoscopy PreparationWhat Is In a Colonoscopy Prep Drink?Colon prep drinks are oral laxatives formulated to flush out the colon. Some brands come in powder form and should be mixed in with water before they are digested. Even liquid prep drinks have to be diluted with water as per the label’s instructions. Different bowel prep kits have various ingredients that work together to induce bowel movement for colon cleansing. One of the leading brands, SUPREP, has sodium sulfate as its primary ingredient. A 6-ounce bottle also contains 3.13 grams of potassium sulfate and 1.6 grams of magnesium sulfate. Another leading brand, PREPOPIK, has sodium picosulfate as its primary ingredient. This active ingredient is known as a stimulant laxative, which induces bowel movement for a successful preparation. Specific ingredients for each colonoscopy prep drink are available online. Regardless of what is in the drink, these kits are specifically designed to fully purge your colon so you can have a successful colonoscopy. How Long Does Colonoscopy Prep Take to Work?Bowel prep medicine should be taken at least 24 hours before the procedure to ensure that the colon is clean prior to the exam. On average, preps take an hour to three hours to work, depending on the brand. A follow-up taken at a much weaker dose is commonly recommended to patients who don’t experience anything after drinking the medicine. Keep in mind that not all patients will respond in the same way as others; give the medicine some time before drinking more of the recommended dose. Diarrhea is a clear indication that the prep is working. Patients can tell their colon is empty when clear yellow liquid comes after passing waste. This means that the colon has been thoroughly cleaned and that the prep was successful. If nothing happens five hours after drinking the prep, it’s best to get in touch with a primary physician to get advice on what to do. Do You Have to Drink All the Colonoscopy Prep?Not necessarily. Depending on the time of your exam, the full solution can be ingested throughout a 2 hour period or twice in between 12 hour intervals. Below are our recommended steps for a successful colonoscopy preparation: Split Preparation: Involves drinking the first half of the solution in the evening and the other half in the morning. This is ideal for patients with colonoscopies scheduled later in the day. 1. Drink the solution at a chosen time. We recommend starting no later than 6 PM. 2. To make the prep more manageable, consume the drink slowly over the course of two hours. Drink the solution in 10 to 20 minute intervals. 3. Be careful not to consume the entire half of the solution in under an hour. Likewise, it won’t be as effective when taken for more than 2 hours. 4. Drink recommended liquids until the colonoscopy to stay hydrated. Full Day Preparation: Best done for patients with colonoscopies scheduled early in the day. Drink the entire solution over three hours one day before the colonoscopy. 1. Drink the solution at an early time. We recommend starting before 6 PM. 2. Consume the solution slowly in 10 to 20 minute intervals over the course of three hours. 3. Be careful not to drink the solution for more than 4 hours. Finish the preparation and drink clear liquids to stay hydrated. Types of Colon Prep DrinksVarious prep drinks are available on the market. Below are our recommended brands for colonoscopy preparation:
Plenvu: New One-Liter Colon Prep DrinkHigh volume prep drinks have always been the norm. However, a brand new liquid drug called Plenvu is posing to replace traditional prep drinks. Uncomfortable preparation is the number one deterrent of colonoscopy screening. Plenvu, on the other hand, is a “lower-volume, one liter bowel preparation”. With lower-volume alternatives such as Plenvu rising on the market, patients can have a more comfortable preparation, which could encourage more patients to get screened for colon cancer. Things to Do Before Your Colon Prep5 Days Before Colon Prep: Change Your DietSwap foods for a low-fiber, low-fat diet. Suitable foods include:
The idea is to only eat foods that are easily digestible by the stomach. Whole grains, raw vegetables, and other stuff should be avoided days before the colon prep. Other foods to avoid include:
3 Days Before Colon Prep: Switching To Liquid DietAlternate between liquid and solid meals every day leading up to three days before your colon prep. At this point, start increasing your liquid intake while decreasing solid foods. This means incorporating more soup in your diet to help your body get accustomed to a purely liquid diet in the coming days. 1 Day Before Colon Prep: Liquid DietPatients are not allowed to eat any solid food one day before the diet prep. Have drinks, juices, and clear soups ready to keep yourself full. Stock up on medication, wipes, and any other necessities you think will make the colon prep manageable. Your body will not find the strength to go out after a colon prep which is why it’s important to have everything ready a day before you take the prep drink. Clear your schedule for the next day and follow prep instructions as described on the label. What to Expect During Your PreparationPrep periods aren’t a walk in the park. However, knowing what to expect can help you prepare for the process and improve your experience.
Making Sure Your Prep Is EffectiveColonoscopy preparations can be tedious, which is why we recommend doing it right the first time to avoid repetition. Not following the recommended dosage, drinking the solution too fast or too slow, and interference with medication or food are the common reasons why colon preps don’t work. Here are some tips on how to avoid the common pitfalls of colon preps: 1. Vomiting During the PreparationThrowing up during the preparation is one of the top reasons why these kits don’t work. Vomiting the solution prevents the colon from fully absorbing the drink. This means that the colon won’t effectively expel waste in preparation for the exam, preventing the examiner to clearly see the lining of the colon. Tip: Drinking the colon prep without throwing up is completely achievable. Take an anti-nausea medicine to ease queasiness. Drink the solution slowly, preferably with a straw, to keep yourself from feeling sick. Take short but frequent breaks in between sips. Following up with a glass of cold water can also help keep the stomach under control. What Happens When I Throw Up During Prep?The solution has to make its way down to the colon to work. Without the full dosage, the colon will not be efficient in expelling waste, making it impossible for the colonoscope to properly observe the colon. Signs of the prep working usually manifest an hour after drinking a suitable amount of liquid. When feeling sick, it’s crucial to prevent the liquid from being expelled orally. Stop consuming the drink until nausea and vomiting have subsided. We recommend taking a break for 30 minutes before drinking any more of the liquid prep. 2. Drinking the Solution Too Fast/ Too SlowNot consuming the recommended dosage can lead to inaccurate results and a stressful prep. All preparation kits, no matter what the brand, include an instruction guide to ensure that patients go through the process as closely as possible. By adhering to the instructions, patients can maximize their comfort while ensuring that their colon is effectively clean for the examination. Can You Drink Colonoscopy Prep Too Fast?Drinking too much of the solution in one go can shock your body. When this happens, too much water is pulled into the colon, leading to very watery stools. Stomach cramps can also come as a result of drinking your prep too fast. Rushing the prep may trigger the gag reflex and induce vomiting. As discussed, most preps are best taken in 10 to 20 minute intervals, over the hours of two hours, or whichever the recommended time is on a chosen brand. 3. Not Drinking Enough Of The Solution Some patients are convinced that clear stools are a sign of a successful preparation, leading them to abandon the rest of the colon prep drink. In reality, clear stools don’t guarantee that the procedure is foolproof. Because of this understanding, patients fail to follow the recommended dosage, at the expense of having an efficient colonoscopy. Can You Stop Drinking Colon Prep When Stools Are Clear? No. Prep is only considered done once all of the prep drink is consumed. Passing clear liquid stools could only reflect the cleansing of the lower part of the colon. It takes a while for the liquid to expel waste from the entire colon, which is why it’s important to finish the entire colon prep drink. Consume the rest of the liquid even if you are already passing clear liquid stool. Drink other clear liquids to stay hydrated throughout the process. Not only does it prevent dehydration, but it also helps clean out cloudiness in the colon. Making The Drink More Manageable Keeping the drink down is one of the most important parts of the prep. Lucky for patients, there are different ways to make colon prep drinks more palatable. Here’s how: Can You Add Flavoring To Colonoscopy Prep? Definitely. In fact, some preps already come with various optional flavorings that can be added to make the drink easier to swallow. However, for mixes that don’t include any flavoring, low-calorie and sugar-free beverages can be added for extra help. Choose a powdered beverage mix that is colorless and easily soluble in cold water. Common options include a Crystal Light packet and apple juice. Ask your physician before adding in any sugar or sugar substitutes. On the other hand, any form of dairy can’t be added to the prep. Avoid anything with red or purple color since these may be interpreted as blood on the colon lining. What Can You Mix With Colonoscopy Prep? Dissolving the prep in chilled water is a common practice. However, it’s also possible to dissolve the colon prep powder in a sports drink or clear juice. When mixing with liquids other than water, take into consideration sugar level and electrolyte presence. Constant bowel movements are bound to make any patient weak, so it’s important to ensure that the liquid and electrolytes lost are restored through drinking liquids in large amounts. Drinks like Gatorade G2 are a perfect vessel for a prep drink. When in doubt, contact your primary physician and make sure that your mixer won’t interfere with the preparations. Signs The Colon Prep Drink Is Working 1. Progression In Bowel Movements The bowels are meant to change after drinking the solution. Expect initial bowel movements to be composed of firm to semi-firm stools. As the colon takes up more liquid and expels more waste, the stools will be liquid in consistency and clear in color. Keep drinking water or other clear liquids to aid in the cleansing. 2. Bloating and Cramping Although uncomfortable, bloating and cramping are both good signs that the prep is working. As the colon pulls in water to expel waste, your stomach can get triggered, causing irritation and pain. This results in bloating and cramping in the abdominal area. 3. Clear brown liquid As more and more fecal matter is expelled from the colon, your colon will start expelling waste in the form of clear brown liquid. Don’t be alarmed: at this point, the bowel movement will start slowing to a halt until no waste is present in the colon. 4. Yellow clear liquid Expelling yellow clear liquid is a clear sign that the prep has worked successfully, and that the colon is clear from majority of the waste. This can happen before all the liquid prep has been consumed. When it does, keep drinking the solution until the entire prep kit has been consumed. Otherwise, the cleanse would not be as effective. Reducing Discomfort During Preparation Why Is It Uncomfortable In The First Place? It’s not just the process of drinking the actual solution that makes the prep so uncomfortable. Physical pain is often reported by patients as a result of frequent bowel movement. Here are the two most common complaints when it comes to colon preparations:
Helpful Tips For An Easier Colon Prep 1. Keep the solution cold. Keep the drink above room temperature to make it easier to swallow. Freeze the container the night before the colon prep or simply refrigerate the mix. Adding ice cubes after mixing the prep powder in water will dilute the drink and lessen its effectivity. 2. Set your pace. Some patients prefer to chug their prep while others prefer to use a straw. Take your time and drink depending on your comfort level. The important thing is to drink each and every drop of the liquid, regardless of how you do it. 3. Make dietary modifications. As discussed, make changes to your diet days before the colon prep. This adjustment allows for an easier colon cleansing and a more comfortable colon preparation. 4. Hold out on the spice. Spices can irritate your anus during consistent bowel movements. Avoid spicy foods up to 3 days before your colon prep. 5. Keep medicine in hand. Nausea medicine is a necessity for patients who have trouble keeping the drink down. Ask your physician in advance regarding drug interactions between your chosen prep drink and the anti-nausea medicine. 6. Get some clear juices and soup. Refuel your body with approved drinks and food. This includes clear juices like apple juice and broth and bone-based soups. When picking out drinks, choose those with electrolyte to keep your systems in balance. 7. Plan your first meal. Hunger, fatigue, and nausea can make any colonoscopy preparation challenging. Set your first meal in mind as a goal to keep yourself focused throughout the preparation. 8. Keep entertainment ready. Preps can feel long and arduous so make sure to keep entertainment ready. Use this time to catch up on a show, watch a new movie, or finish an old book. 9. Use flavorful juices as mouthwash. When the flavor of the prep gets too overwhelming, use clear juices to fight the flavor by using it as mouthwash. Swish the juice around your mouth for a couple of seconds and spit it out. Repeat frequently to prevent vomiting during the process. 10. Ask around for alternatives. Aware of certain complications? You may request a different kind of bowel prep if you think the one prescribed to you won’t work. There are dozens available on the market, from powder to pill form, to generic to branded. Liquids and Colonoscopy: Diet, Hydration, and What To Avoid What Is A Clear Liquid Diet? Patients are kept on a clear liquid diet to ensure that the colon doesn’t have any residue or waste. Normal foods leave particles and residue that may affect colonoscopy reports. The rule of thumb for this diet is making sure the food is clear; as long as you’re able to see through the food, it is considered a clear liquid diet. These foods include:
Liquid diets are limited precisely because they are not meant to be palatable. The purpose of the diet is to maximize the prep drink, while keeping the body hydrated. Liquids limit the strain on the intestine and keep the body up and running even without significant nutrients. Liquid diets are only recommended for tests and should not be extended beyond the necessary timeframe. Patients will be allowed to resume regular meals once the colonoscopy has been completed. Liquid Diet Sample Listed below are some ideas on what a clear liquid diet looks like:
Frequently Asked Questions What do you drink before and after a colonoscopy?
Can you drink alcohol before a colonoscopy?
Can I drink coffee before a colonoscopy?
What juices are allowed before a colonoscopy?
Are all kinds of gatorade allowed before a colonoscopy?
Are There Alternatives To Colonoscopy Prep Drink? There are no other ways to clean out the colon except by drinking a colon prep drink. With many options available, you are bound to find one that works best for you.
However, doctors say that patients should be wary with low-volume preps. While convenient, there is no recognized study stating that low-volume options are just as good as high-volume ones. As gastroenterologist Dr. Michael Bernstein said in a report, “The downside is that it doesn’t tend to be quite as good at cleaning out the colon.” Colonoscopy preparations may be inconvenient, but they are nothing compared to having to fight actual colon cancer. Get in touch with us today to learn how we can make your colon prep comfortable. The post Colonoscopy Prep Drink: A Complete Guide for a Joyous Colonoscopy Preparation appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/colonoscopy-prep-drink-a-complete-guide-for-a-joyous-colonoscopy-preparation/ Colonoscopies are hailed as the golden standard for colon cancer screening. Praised by many as life-saving, more and more physicians are recommending colon cancer screening for everyone, even patients that are considered low-risk. Are colonoscopies necessary for everyone? Not at all. Only individuals who qualify as high-risk are recommended to have regular screening, and even then, physicians will recommend a schedule that normally doesn’t go beyond once every three years. Understanding the purpose of colonoscopies and who needs them the most is key to determining whether or not the test is relevant to your health. What Are Colonoscopies For?A colonoscopy is a medical examination involving a device called a colonoscope. This device is long and is typically made from a thin, flexible plastic with light and camera attachments at the end. There are three reasons why colonoscopies are performed:
Colonoscopies are used to diagnose and treat a host of gastrointestinal abnormalities, with colon cancer being the major concern especially for adults 50 and older. A study from the American College of Physicians affirms how necessary it is to perform routine colonoscopies, showing a 61% decrease in colorectal cancer mortality among veterans under the Veteran Affairs health program. What Can Colonoscopies Detect?
Deviant cell behavior can lead to polyp growth along the colon lining. With a colonoscopy, doctors can see, remove, and test the polyp to rule out colon cancer. But that’s not the sole function of a colonoscopy. It can also be used to look for:
What Are the Signs You Need a Colonoscopy?Inflammations, infections, and abnormal growths along the digestive tract produce a variety of symptoms. When these signs occur, physicians recommend a colonoscopy to reach a definitive diagnosis. Here are some things to watch out for:
Colonoscopy, Aging, and RisksThe Link Between Aging and RiskThe National Foundation for Cancer Research states that 90% of colorectal cancer cases appear in adults ages 50 and older, with the average age of diagnosis at 64. Colon cancer is so prevalent in older individuals that 1 in 4 people will have polyps on their colon by the time they reach 50 years old. Older adults are at a higher risk of developing colon cancer, or any cancer for that matter, because cell generation slows down with age. Add to that the body’s exposure to alcohol, cigarette, and unhealthy dietary choices during the younger years. This “older” environment makes it impossible for the body to continually expel unhealthy cells and replace them with new ones, making it conducive for abnormalities to develop at the molecular level. At What Age Do You Need a Colonoscopy?The original screening age recommended by the American Cancer Society was 50. Revisions were made due to recent developments concerning rising incidents of colorectal cancer in younger adults. The current recommended screening agehas been lowered to 45. This means that adults aged 45 and above are eligible for a free colonoscopy screening, depending on their insurance plan. I’m Younger Than 50. Do I Need a Colonoscopy?People aged 45 years old are now considered at an average risk of developing colon cancer due to recent findings. New research found that colorectal cancer is increasing in both young and middle-aged adults in the US. For adults aged 20 to 39, the lifetime risk of developing colon cancer has increased up to 2% every year from 1990 to 2013. Another study revealed that about 11% of colorectal cancers are diagnosed in adults aged 50 and younger. Although old age remains to be a primary risk in developing colon cancer, the consequences of poor lifestyle choices can also manifest earlier in the form of polyps along the colon lining. Excessive smoking, eating, and a sedentary lifestyle can all lead to greater risk of developing cancer at an early age. Am I at Risk for Colon Cancer?Other circumstances unrelated to age may increase the risk of developing colon cancer. These include:
Individuals who are considered at a high risk of developing colon cancer are recommended to get a colonoscopy. For average-risk individuals, the recommended frequency is once every ten years, and at least once every two years for those at an above average risk. Do You Need a Colonoscopy?
Too much of everything can cause problems in your body, and that includes the golden test for colon cancer screening. Diligent screening can prevent cancer and save lives, but too frequent testing is unnecessary and could even cause complications. Although uncommon, colonoscopies can pose a number of risks when performed unnecessarily:
When Is Colonoscopy Warranted?Individuals who test negative during a colonoscopy (meaning no polyps were found), have healthy lifestyle choices, and have no pre-existing conditions that may influence polyp growth are considered low risk. They are recommended to undergo another screening after ten years. Anything outside that is considered too intrusive for the colon, which may lead to complications. On the other hand, individuals with detected or removed polyps are recommended to have their next colonoscopy within 5 to 10 year’s time. This also applies to individuals who are over the age of 45. We recommend communicating with your gastroenterologist to find out the best colonoscopy frequency specific to your health. Colonoscopy: Life-Saving Or Bank-Breaking?Are Colonoscopies Over Prescribed?Needless medicine prescription, specifically antibiotic, is not new. New reports found that about 30% of tests suggested by doctors are actually unnecessary, with colonoscopies being one of the more targeted tests. It’s sensible for doctors to schedule a follow-up colonoscopy. However, it’s unnecessary to do follow-ups earlier than the guidelines set by the American Cancer Society. Once every ten years is the ideal frequency for those at an average risk, while 1 to 2 times every two to five years depending on the case is recommended for those who are predisposed to the cancer. As mentioned above, unless you qualify as a high risk individual, there’s absolutely no reason to test more than once every ten years. Lead author Dr. Gina Kruse says that colonoscopies are overused and appeal to patients to be more conscientious regarding recommended tests. When Not to Have a Colonoscopy?Out of pocket colonoscopy costs can go up to $10,000 in major cities. Avoid necessary costs by understanding when not to have a colonoscopy. This is applicable when:
When Are Colonoscopies No Longer Necessary?The good news is that colon cancer risk decreases for people aged 75 and older. This guideline is set by the U.S. Preventive Services Task Force (USPSTF) together with the American College of Physicians (ACP) after determining lower incidence of colon cancer in people within this age group. This doesn’t apply to patients who are at a high risk. Even at this age, those who were previously diagnosed with polyps or colon cancer have to continue surveillance in order to prevent recurrence. ConclusionUnless diagnosed with a polyp or colon cancer, it’s important to treat colonoscopies like any other tests: as preventative measures. When done right, this test can catch colon cancer or even growths before they evolve into cancer. Stick to the guidelines recommended by various health institutions to ensure that every colonoscopy is beneficial to your health. Are you ready to get a colonoscopy? Book a consultation today. The post Is Colonoscopy Necessary for Everyone? appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/is-colonoscopy-necessary-for-everyone/ How Much Does a Colonoscopy Cost?Colonoscopy costs vary depending on a number of factors. Colonoscopies can cost anywhere from $2,000 to $10,000 for patients without health insurance. On the other hand, those getting screened with health insurance typically have $1,000 deductible on average. Why Do Colonoscopy Costs Vary?The final cost of a colonoscopy can depend on different variables. Prices vary because of the following factors:
Breaking Down the Colonoscopy BillA colonoscopy procedure involves a couple things, including the test itself. Other charges will be reflected on your final cost, which includes the following:
Insurance Coverage for Colonoscopies: Private and MedicareColonoscopies are the most expensive screening tests afforded by Americans. Data suggests more than 10 million people get screened for colon cancer annually, which adds up to $10 billion in yearly costs for colonoscopies alone. In an effort to lower the colon cancer mortality rate, the United States Preventive Services Task Force (USPSTF) strongly recommends proactive colonoscopy screening to all Americans. To incentivize more individuals to get screened for colorectal cancer, a federal law has been passed to reduce out of pocket costs for colonoscopy. The Affordable Care Act and Colonoscopy CoverageAs previously mentioned, the Affordable Care Act (ACA) mandates Medicare as well as private insurers to cover all costs for preventative colonoscopy screening. However, this doesn’t mean that all colonoscopies are completely free of charge. Discussed below are some nuances of colonoscopy coverage:
How Can I Get a Free Colonoscopy?The Affordable Care Act (ACA) makes it possible for patients to get a free colonoscopy under certain conditions. Recent studies showing the rising incidence of colon cancer in young adults as young as 35 has pushed the American Cancer Society (ACS) to make amendments in their recommended screening age. With this, the ACS has changed the recommended screening age from 50 to 45. This means that individuals with a familial history of colon cancer, alongside those who are at an individual risk due to the presence of other gastrointestinal syndromes and general medical conditions, may qualify for a free colon cancer screening at an earlier age. Online tools can help patients understand if they are eligible for free colon cancer screening. This website offers a free quiz to help identify if you are eligible or not. Note that these materials don’t guarantee a free colonoscopy. We recommend that you get in touch with your insurance provider and facility of choice to get an accurate colonoscopy cost. Frequently Asked Questions1. Does My Insurance Cover Colonoscopy? Patients undergoing a colonoscopy for the first time are likely to be eligible for a free test. Patients who are not exhibiting common colon cancer symptoms are considered healthy, and as such the colonoscopy will be defined as a preventative measure against cancer. For patients who are exhibiting symptoms or are at high risk of colon cancer, there is no definitive way of telling if you are eligible for a free colonoscopy. We recommend that you ask your insurance provider about the specific cost of your test, and whether it will be fully or partially covered by your current plan. For Medicare holders, colonoscopies are fully covered once every 10 years for average-risk individuals and every 2 years for high-risk patients, regardless of age. 2. Getting A Colonoscopy Before 50 90% of colon cancer cases are detected in individuals age 50 years and older. However, recent cases of colon cancer in younger adults have paved the way for more lenient screening rules, leading to more inclusive policies for younger plan holders. Even then, different health plans offer varying benefits. Some providers may allow full or partial insurance coverage for individuals within the 45-49 range, while others may choose to keep their colonoscopy cost-free exclusively for patients 50 years and older. 3. At What Age Does Medicare Stop Covering Colonoscopy? Medicare holders are reimbursed for colonoscopy regardless of age. A study published in the Annals of Internal Medicine suggest that colonoscopies may not even be necessary for adults over the age of 75, since the risk of developing colon cancer is reduced in patients aged 70 to 79. Although the overall lifetime risk is reduced, individual health also plays a factor in the risk of developing colon cancer. Patients with type 2 diabetes, for example, may still develop colon cancer later in their lives. 4. Is Colonoscopy Preparation Covered By Insurance? The actual colonoscopy is only a part of the screening. Prior to the actual examination, patients will be asked to go through a colon prep. This involves the ingestion of a substance designed to clean the colon to ensure accurate test results. In some cases, patients may also undergo a pre-test consultation, and is not necessarily covered in the policy. This means that bowel preparation kits, costing anywhere from $9 – $120 depending on your prefered kit and coverage plan, are not fully covered by insurance companies. Top Bowel Preparation Kits and Cost
5. What Counts As Routine/Preventative Colonoscopy? Colonoscopies are only free when classified as preventative. It’s safe to say that anyone undergoing a colonoscopy for the first time is eligible for a free test. On the other hand, colonoscopies may be considered diagnostic or medical in nature under the following conditions:
6. I’m Scheduled To Have Another Colonoscopy. Is It For Free? Patients who have received full coverage for their previous colonoscopy but have undergone polyp removal are no longer eligible for a free colonoscopy. At this point, the test will be classified as surveillance screening rather than diagnostic in nature due to the previous discovery of polyps in the colon. Deductibles and copayments depend on your provider. Learn more about your plan in order to understand its full benefits. 7. Is Anesthesia Covered For Colonoscopy? The U.S. Department of Health and Human Services (HHS) issued a notice in 2015 clarifying anesthesia coverage for colonoscopies. This states that insurance providers, both private and government-provided, may not impose extra costs for anesthetic services, as long as they are done for preventive colonoscopies. Copayments and deductibles are usually applied to patients undergoing colonoscopies after a polyp has been detected. This also applies for colonoscopies done to prevent the recurrence of colon polyps. Getting the Most Out of Your ProviderFor Patients with a Family History of Colon CancerIn some cases, insurance providers may cover free testing for individuals with a proven family history of colon cancer. We recommend doing the following in order to increase your chances of qualifying for a free colonoscopy: 1. Find out if you have a first-degree relative who was diagnosed with either colon cancer or polyps before the age of 50. 2. Make a record with your primary physician. This declaration will show up in your medical records, noting that you have a family history of colon cancer. This will include the relative’s name and his or her age during the diagnosis. 3. Ask about screening benefits from your insurance provider. Use your medical record as proof for being at an above average risk for colon cancer. Note that this should be done before you schedule a colonoscopy since benefits are not guaranteed and vary depending on your plan. Questions to Ask Your Insurance ProviderHealthcare policies are rarely straightforward, making it difficult for the average patient to really understand the full extent of his or her benefits. Asking your provider beforehand allows you to prepare financially before the colonoscopy bill rolls in. Here are some questions you should ask in preparation for a colonoscopy:
Out Of Pocket Colonoscopy Cost$2,000 and above is the common out of pocket cost for uninsured patients in the U.S. However, there are various options available online and locally that could help mitigate colonoscopy costs. Check For Local Programs In Your AreaSites like Colonoscopy Assist help patients all over the U.S. find cheaper colonoscopies in their areas. With various programs available in over 25 states, uninsured patients can pay as low as $1,075 for an all-inclusive screening. You can also ask around public health organizations for ongoing programs that help uninsured patients get lower costs for their colon cancer test. Get a Colonoscopy LoanPersonal loans can be used to fund a colonoscopy. The same rules for taking out a personal loan apply when being used for medical reasons. Get in touch with your bank or private lender to learn the specifics of their lending policy. Are Colonoscopies Worth It?A colonoscopy may be expensive, but it’s nothing compared to actual cancer treatment. In 2014, the American Cancer Society published the out pocket costs of cancer patients: a staggering $4 billion. Through the years, colonoscopy has remained to be the golden standard in colon cancer screening, and for good reason. At the end of the day, the minor financial and logistical inconveniences posed by colonoscopy are actually privileges when compared to the relentless costs and stress from late stage colon cancer. When it comes to colon cancer, time is money. Book a colonoscopy today. The post The Cost of Colonoscopy: Insurance, Anesthesia, And More appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/colonoscopy-cost/ Undergoing a colonoscopy can be a nerve-wracking affair. It’s common knowledge that colonoscopies can be uncomfortable, especially for first-timers. This makes a lot of people averse to getting screened, even though they are at high-risk for colon cancer. In reality, not all colonoscopies have to be uncomfortable. Your level and type of sedation or anesthesia is an important choice to make, and can define your colonoscopy experience, the recovery, and side effects afterwards. Understanding the specifics of anesthesia for colonoscopy is crucial towards making the right choice for yourself. What is a Colonoscopy?A colonoscopy is a medical procedure that involves a colonoscope, a medical device that consists of a small camera and light mounted on a thin, flexible tube. The tube is inserted into the patient’s rectum and pushed up into the large intestine, also known as the colon. The procedure is invasive in nature. In some cases, doctors introduce air into the colon to gently inflate it, allowing them to see better. Patients may experience discomfort after the exam because of this. The minor inconvenience posed by colonoscopies are mitigated when its benefits are considered. This procedure can save a patient’s life by effectively detecting and removing polyps, which increases your chances of preventing or even surviving colon cancer. Why Do Patients Need a Colonoscopy?Patients are recommended to get a colonoscopy if they are experiencing symptoms such as:
These symptoms can be signs of colon and colorectal cancer, which can develop in patients who have some or all of the following risk factors:
While many people associate colon cancer with patients 50 years and above, colon cancer can actually develop at any age. If doctors observe symptoms similar to those listed above, you may be recommended for a colonoscopy regardless of your age. Colonoscopy and Anesthesia: Everything You Need To KnowAs a patient, you have the right to decide on the level of sedation and the type of anesthesia for your colonoscopy, so it is important for you to understand the varying levels of colonoscopy sedation and what anesthesia colonoscopy can do to your body. Levels of Colonoscopy SedationFirstly, it is important to be aware of the different levels of sedation that you can be under while undergoing a colonoscopy.
There is a very low risk of any interference with the body’s cardiovascular function. However, one noteworthy effect is the lack of memory: patients under moderate sedation generally have little to no memory of it.
Many patients generally ask to be unconscious for a colonoscopy, but after they are informed of the potential risks of general anesthesia, patients generally opt for a lower level of sedation instead. Sedation Levels: Which to Choose?Every level of sedation has their own set of advantages and disadvantages. Here are the different experiences you may undergo with each level of sedation: Sedation LevelsNo Sedation – Best For No Downtime: While not many patients choose to undergo a colonoscopy without any sedation, patients who do choose this path have the quickest recovery after the procedure. They have very little recovery time and can operate at normal levels immediately afterwards. They also do not have to worry about possible anesthesia-related complications. If you decide to undergo a no sedation colonoscopy, discuss this possibility with your doctor and make sure that they have done unsedated colonoscopies in the past. Light Sedation – Not Recommended: A rare choice of sedation level, as it carries the risk of anesthesia complications without offering many of the benefits of sedation. Patients will not be able to participate in daily activities until at least the day after their procedure. Moderate Sedation – Reliable Choice: The most common sedation level with the colonoscopy procedure. Here, patients are generally given fentanyl (a pain killer) and midazolam (a sedative, mild). To make sure that the patient has the right amount of sedation, a nurse and doctor should monitor the patient during the entire procedure and sedation duration. Deep Sedation – Requires Anesthesiologist: Deep sedation can also be referred to as MAC, or Monitored Anesthesia Care. Propofol is the top choice of sedation for this sedation level, and it is administered by an anesthesiologist as well as your doctor and nurse. General Anesthesia – Rare: Very rarely used for colonoscopy, and is only recommended for patients who have issues with their lungs or will experience longer examinations. The Colonoscopy Patient Anesthesia ExperienceYour experience of anesthesia and sedation during a colonoscopy will depend on the type of anesthesia you choose, however you can expect a general experience if you choose moderate sedation or deep sedation, in which an anesthesiologist is present. Prior to your procedure, your doctor should prepare you with instructions for the days leading up to your colonoscopy. These are meant to make sure that your colon is empty. For anesthesia, it is best that a patient avoids drinking clear liquids for two hours before the examination, and avoids eating any food for eight hours before it. When you come in for your colonoscopy, a nurse and an anesthesiologist will discuss with you your vital signs, medical history, and any potential problems you might have with the anesthesia. If you have serious potential problems, you will be recommended to take conscious sedation instead of heavier sedation levels. Patients with no problems with their blood pressure or heart will have an intravenous drip attached to their arm. In about five minutes, the patient should be unconscious from the anesthesia. Patients are generally surprised to wake up later and find out that the procedure is done. FAQ – Colonoscopy and AnesthesiaWhat kind of anesthesia is used for colonoscopy? Is colonoscopy done under general anesthesia? This depends on the type of anesthesia or sedation level the patient chooses. Generally, the sedative agents for colonoscopy include Propofol, midazolam, and fentanyl. How long does colonoscopy anesthesia last? After a colonoscopy, a patient can expect to stay at the hospital or a recovery room for up to two hours after the examination. However, a patient will not be fully recovered from the anesthesia until up to 48 hours after the procedure. How painful is a colonoscopy without sedation? While many patients are fearful of the idea of undergoing a colonoscopy without sedation, several studies have found that it isn’t as painful as many believe. In one study, 73% of patients who were given an unsedated colonoscopy were willing to do it again. How long does a colonoscopy with anesthesia take? The entire colonoscopy procedure should take anywhere from 30 minutes to an hour. Why is an anesthesiologist necessary for anesthesia? When dealing with Propofol, the main sedative for colonoscopy anesthesia, the Food and Drug Administration has made it a requirement that a nurse anesthetist or anesthesiologist must be present during drug administration. This is because Propofol can lead to apnea and other side effects. Possible Side Effects of Colonoscopy AnesthesiaAnesthesia with colonoscopy has become a topic for debate in the medical community due to the possible side effects, risks, and complications experienced by patients even at the conscious sedation levels. These side effects include: Respiratory Depression: Respiratory depression is the condition that occurs when a patient experiences fewer than 12 breaths every minute. Their breaths become ineffective, slow, and shallow, due to the strength of the sedative in slowing down the brain signals that deal with breathing. The mild anesthesia popular with colonoscopy examinations has been found to occasionally affect the respiratory drive. Bradycardia: Bradycardia, or slow heart rate, can be caused by the effects of anesthesia on the autonomic nervous system. The autonomic nervous system (ANS) is responsible for body functions such as the heart rate, and bradycardia can be potentially dangerous to some patients with weaker hearts. Hypotension: Hypotension, or low blood pressure, leads to dizziness, fatigue, and overall feelings of exhaustion. Anesthesia in colonoscopies has been found to lead to hypotension, which is why anesthesiologists should first check patients who regularly take medication for their blood pressure. Vomiting, Nausea: Vomiting and nausea are common side effects of pain relievers and sedatives. This is why patients are prohibited from eating or drinking for several hours prior to a colonoscopy. Colonoscopy With Anesthesia: Is It Necessary?More patients are considering alternative options before undergoing a full anesthesia for a colonoscopy. Is full anesthesia right for you, with costs, pain, and alternative treatment options considered? 1) Anesthesiologists Might Not Be Covered By Insurance The costs associated with anesthesia can sometimes be much more than most patients would expect. The main issue is that anesthesiologists are often not covered by general health insurance plans, meaning patients have to pay out of pocket for a simple anesthetic. Some gastroenterologists also recommend that patients undergo full anesthesia for a colonoscopy, however there is little scientific evidence showing that it is necessary. In many cases, patients might prefer to forego anesthesia altogether after finding out how much it will cost. 2) Not As Painful As You Might Think Many studies have found that the pain of an unsedated colonoscopy is actually within the pain threshold of most patients. While the sensation may be an unusual and uncomfortable sensation, a majority of patients studied by researchers claimed that they would undergo the procedure without sedation again. 3) Alternative Tests For patients who are adamant against the colonoscopy procedure and dealing with anesthesia, there are a few alternative tests they may consider. The best alternatives to colonoscopy include:
While alternative tests can be easier on the patient, note that they are not as effective as colonoscopy. Additionally, alternative tests may be able to identify and locate polyps and colon cancer, but a colonoscopy will still be necessary afterwards for the actual removal. Learn More About Colonoscopy AnesthesiaFor individuals interested in learning more about colonoscopies, anesthesia, and safe and proper anesthesia practices, feel free to contact us at the Gastro Center in New Jersey. We are always ready to assist patients in understanding more about their needs and concerns. Contact us today and learn about how we can help you and your upcoming colonoscopy. The post Colonoscopy Anesthesia: Types, Levels, and Possible Side Effects appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/colonoscopy-anesthesia/ Hemorrhoids and colon cancer are two gastrointestinal complications that are on opposite ends of the spectrum. One is a common, curable inflammation; the other is notorious for high mortality rates in the United States. Despite the differences in the nature of the diseases, people often mistake one for the other, which can prove detrimental especially if colon cancer symptoms are treated like hemorrhoid symptoms. So how is colon cancer different from hemorrhoids? Colon cancer is a fatal cancer that mutates from abnormal polyp growth, while a hemorrhoid is an inconvenient yet temporary inflammation around the rectum area. Sometimes their symptoms may overlap, but it’s important to understand that hemorrhoid symptoms eventually recede and get better, while colon cancer only further mutates and spreads throughout the body. What Are Hemorrhoids?Hemorrhoids are swollen blood veins growing along the lining of the lower part of the rectum and anus. They can either grow internally, above the rectum’s “exit” point, or grow externally where it is visible during an examination. Although common, the nature of this condition makes patients averse to discussing it openly. Roughly 1 in 20 people are diagnosed with hemorrhoids in the United States. Studies show that about half of adults 50 years of age and older are likely to be diagnosed with hemorrhoids. Pregnant women are also susceptible to hemorrhoids due to changes in the uterus (source). CauseThere are no definite reasons why hemorrhoids exist. However, doctors believe that straining during a bowel movement, prolonged sitting (especially on the toilet), and constipation can all aggravate symptoms. Extra pressure on the anal canal can trigger painful inflammations. The muscles along the walls of the rectum can enlarge and swell. When pressure is applied, the blood vessels inside these muscles blow up, causing hemorrhoids to swell with blood. Here are some factors that could trigger hemorrhoid development:
Types of Hemorrhoids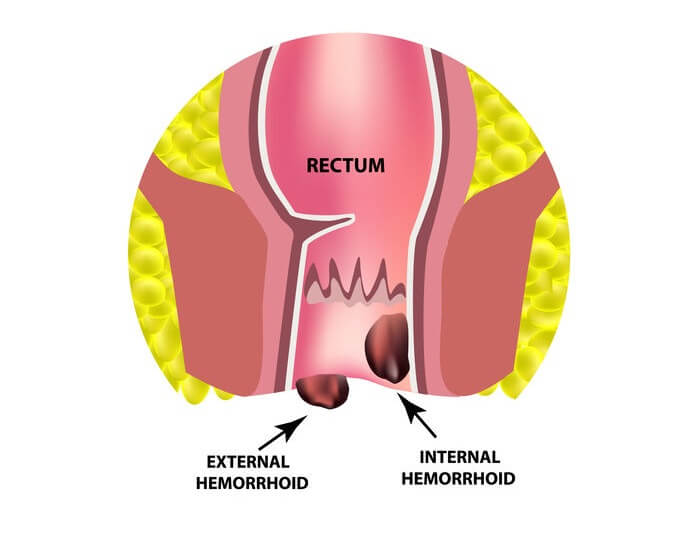
1. Internal Hemorrhoids: This type of hemorrhoid grows inside the rectum and typically grows discreetly unless it gets significantly large. Usually painless, internal hemorrhoids only become apparent because of uncomfortable bowel movement. This type of hemorrhoid may block the stool from passing, which causes blood in the stool. Internal hemorrhoids can protrude outside the anus. In this case, they become visible and painful because of the active nerves around the rectal area. Protruding internal hemorrhoids typically recede on their own. If not, they can always be nudged back into place. This condition is what is known as a prolapsed hemorrhoid. 2. External Hemorrhoids: External hemorrhoids are growths that occur outside anus. These are not to be confused with a prolapsed or protruding internal hemorrhoid. These are usually situated under the skin, and are attached in areas lower than internal hemorrhoids. 3. Thrombosed Hemorrhoids: When aggravated, hemorrhoids can develop a blood clot, causing them to become tender and painful. This development is called a thrombosed hemorrhoid. The growth turns into a purple or blue color due to the absence of normal blood flow. Patients report greater discomfort, itching, and sometimes even pain when sitting. Hemorrhoids that no longer receive any blood flow are called strangulated hemorrhoids. Why Are Older People Likelier to Get Hemorrhoids?Weaker muscles and a sedentary lifestyle are the two main reasons why older people become more susceptible to hemorrhoids. We recommend even 20 minutes of low intensity exercises such as walking, as well as a high-fiber diet to promote good bowel movement. What Is Colon Cancer?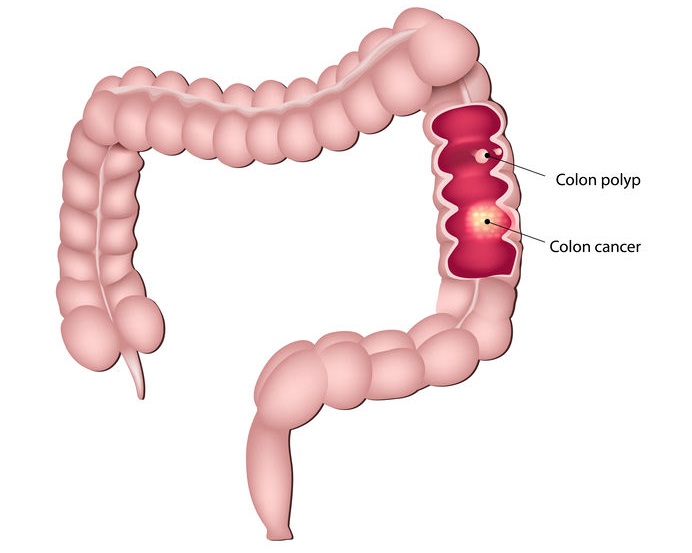
Colon cancer (sometimes referred to as colorectal cancer) develops from polyps or growths along the lining of the colon. It is the third most diagnosed cancer in the United States. According to the American Cancer Society, about 1 in 24 women and 1 in 22 men have a lifetime risk of developing colon cancer (source). CauseCells naturally divide, multiply, and die. However, cell behavior can deviate from normal, leading to an increase in their production and growth. This cellular change creates polyps along the inside of the colon. These growths are what mutate further into colon cancer. Although the main cause for colon cancer is still unknown to scientists, there are risk factors that can increase a person’s chances of developing this type of cancer:
Colon Cancer VS Hemorrhoids: Signs and Symptoms
Bleeding in Colon Cancer VS HemorrhoidsBleeding is a common symptom of colon cancer and hemorrhoids. When people find blood in their stool, they often immediately assume it’s one or the other since this is a commonly seen symptom. While true, there are slight differences in the bleeding caused by colon cancer compared to what is caused by hemorrhoids. It is important to understand that colon cancer and hemorrhoids occur on two different areas of the gastrointestinal tract. Hemorrhoids, both internal and external, grow at the lower part of the tract, just a few inches away from the anus. Colon cancer, on the other hand, is caused by polyps found in the ascending colon (“left colon”) or descending colon (“right polyp”), in the upper part of the tract. Some anatomical knowledge makes it easier to understand the difference between bleeding caused by either abnormalities. Hemorrhoid BleedingHemorrhoid-induced bleeding is caused by the stool rubbing against the hemorrhoid as it passes through the rectum. In some cases, the hemorrhoid itself bleeds and may make its way down the rectum. However, it’s more common for stool to bump against obstructive growth, causing it to rupture and bleed. The bright red blood comes from how “fresh” the wound is. The bright red blood patients report is the stool rubbing against an inflamed hemorrhoid. Colon Cancer BleedingContrary to popular belief, the presence of blood in the stool is not always a sign of colon cancer. In fact, colon cancer symptoms gradually develop over the course of 10 years, and only ever begin to appear in its later stages. Colon cancer itself doesn’t cause internal bleeding. The blood in the stool reported by patients is the polyp bleeding after it gains significant mass. Instead of bright red blood, diagnosed colon cancer patients often report dark, tar-like stool. Blood is rarely visible to the naked eye, which is why it’s impossible to detect the cancer just by looking at the stool alone. Are Hemorrhoids a Sign of Cancer?The symptoms for colon cancer and hemorrhoids sometimes overlap, leading patients to believe their hemorrhoid symptoms are actually indicative of polyp growth in the colon. Hemorrhoids and colon cancer are two separate abnormalities. As explained, hemorrhoids occur when extra pressure is introduced in the rectum area, whereas polyp growth occurs only along the colon lining. Can Hemorrhoids Lead to Colon Cancer?100% of colon cancers evolve from large polyps, which are mutated cells that grow along the colon tract. This means that there is zero chance for any hemorrhoid to lead to colon cancer. Again, hemorrhoids are swollen veins on the muscle of the rectum, not mutated cells along the colon. Understand what is causing blood in your stool. Get screened today and reach a final diagnosis. Achieve your peace of mind. The post The Difference Between Colon Cancer and Hemorrhoids appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/colon-cancer-hemorrhoids-difference/ 90% of colon cancer cases in the US are diagnosed in patients 50 years old and older. However, recent studies show a rising incidence of colon cancer in younger adults. Bowel cancer found in ages 20 – 30 rose between 1990 and 2016, increasing as much 7.9% per year between 2004 and 2016 (source). With various screening options available, logistical and financial barriers no longer stand in the way of getting screened. One of the most popular options is at-home colon cancer screening tests. But just how effective are they? Colon cancer screening kits can have an accuracy rate of up to 92% with only a 5% chance of false-positives. With something this affordable and accessible, medical practitioners are hoping to see a consistent drop in mortality rates caused by colon cancer. And with at-home colon cancer screening tests, patients no longer have to go out of their way to get tested. The Importance Of Colon Cancer Screening
Survival rates of colon cancer patients are significantly higher when the disease is still in a localized stage. Within five-years, patients in this stage have a 90% chance of survival. This gets lower as the cancer spreads throughout the body. Colon cancer evolves from polyps, which are growths on the lining of the colon. When caught early, these polyps can be removed, preventing them from developing into colon cancer. Getting screened means patients can avoid and even get cured for colon cancer (source). Dr. John Saltzman, who is a director of endoscopy at Brigham and Women’s Hospital in Boston, affirms that: “If you get them at the precancerous phase, they don’t have a chance to grow and turn into cancer.” Why Choose At-Home Colon Cancer Tests
Despite various options for colon cancer screening, even those at an average to high risk don’t get tested until they start exhibiting progressive symptoms. The reason for this is simple: colonoscopies and other procedures are relatively expensive and require a lot of preparation. With at-home colon cancer tests, candidates can get screened and tested in the comfort of their own home. Listed below are other advantages of at-home screening:
Do They Work?
At-home screening is normally suggested to be taken alongside colonoscopies and other methods of testing. A study published in the Annals of Internal Medicine suggests that at-home colon cancer screening, specifically the fecal immunochemical test (FIT) may produce more accurate results than a colonoscopy (source). The lead author notes that the FIT was able to positively identify colon cancer in 75-80% of the individuals. In comparison, colonoscopies are known to have a 95% detection rate. How do these numbers translate in terms of efficacy? Taking into consideration cost and preparation time, patients are naturally averse towards taking colonoscopies for the simple reason that they take time. On the other hand, at-home colon cancer screening doesn’t pose the same barriers. Because they are repeatable and affordable, at-risk individuals can test yearly, which further increases its credibility as a screening method. People with average risk should have a colonoscopy every ten years. It’s important to note that polyps can evolve into colon cancer in 7 to 10 year’s time. But with at-home screening methods such as FIT, among others, patients can test yearly and keep track of their digestive tract health more rigorously. How Accurate Are Home Colon Cancer Tests?
Depending on the test being taken, the accuracy of at-home CRC screening kits can go up to 90%. When taken alongside other screening methods, at-home testing becomes fool-proof. Here’s how it usually works:
Limitations Of At-Home CRC Screening
At-home CRC kits are fully equipped with everything you need to identify either polyps, abnormal cell DNA, or bleeding. We recommend using more than one type to improve the accuracy of your results. While useful in determining pre-cancer warnings, these are not to be treated as definitive diagnosis for colon cancer. Patients who test positive for at-home screening tests are required to take a colonoscopy in order to reach a conclusive diagnosis. Learn more about colonoscopy procedure at Gastro Center NJ. Even with these limitations, At-home kits remain to be useful and potentially life-saving, especially for individuals who are not aware of existing genetic disorders that may increase their risk of developing colon cancer. Vice President of cancer screening at the American Cancer Society, Dr. Robert Smith, even notes that annual at-home testing can be as effective as colonoscopies (source). How Much Do CRC Tests Cost?
In-house screening methods are the last thing from affordable. Colonoscopies can cost up to $3,000. Meanwhile, sigmoidoscopies range from $900 to $2,000. In comparison, fecal occult blood tests (FOBT) can go as low as $4 per test. A more “advanced” kind of at-home testing can cost $8 per test. The Cologuard, which is considered to be the most expensive at-home testing kit, retails at $649. However, that price can still vary depending on the patient’s health insurance. Self-screening kits for CRC are available in pharmacies. These can also be purchased online through Amazon. Consult your doctor for best home colon cancer screening kits available on the market. Choosing the Right At-Home Colon Cancer Test
There are three kinds of at-home colon cancer tests available for use. These are: Cologuard: the only FDA-approved stool DNA test
Cost
Cologuard is covered by Medicare, Medicare Advantages, as well as Medicaid in specific states (click here for the complete list). Cologuard is also in partnership with various private insurance companies. Contact your provider to learn more about deductibles and refundables. Effectivity
Cologuard was able to detect 42% of high-risk precancers and 92% of colon cancers in their study of 10,000 people. The test was also able to detect positive signs of cancer or growth in 13% of people without cancer or precancer. How to Use
Doctors order Cologuard on your behalf. Once the arrangement is done, expect the test kit to arrive at your doorstep. According to the instructions, only one stool sample is required. No dietary or medication changes are necessary. Ship the sample to your chosen lab, as specified in the instructions. Results are sent back in 2 weeks. How It Works
Cologuard looks for traces of blood shed by polyps or growth along the colon lining. More importantly, Cologuard is the only at-home screening kit that can identify abnormal DNA just with stool alone. Guaiac fecal occult blood testing (gFOBT)
Cost
Depending on the brand you choose, gFOBT tests can cost anywhere from $5 to $60. Effectivity
The gFOBT is known to have reduced colon cancer mortalities by up to 25%. How To Use
Patients are provided with three test cards. More test cards may be given depending on race, age, and overall risk factor. Separate bowel samples are collected from separate bowel movements. Be wary of adding water or urine to the sample since this may influence test results. Dietary restrictions are also applicable to preserve the accuracy of the results How It Works
The gFOBT is similar to the FIT in that both tests are able to detect bleeding in the stool. This test uses a chemical indicator that changes in color when blood is present. Fecal immunochemical test (FIT)
Cost
Depending on the brand you choose, FITs can cost anywhere from $10 to $200. Effectivity
FIT is commonly preferred over gFOBT, and has been recommended by the American College of Gastroenterology as the better colorectal cancer detection test. How to Use
No dietary or medical restrictions apply to an FIT. A special device included in the kit is designed to collect the stool onto a collection card. An average of three samples are collected from three separate bowel movements. How It Works
FIT utilizes antibodies in detecting hemoglobin. If hemoglobin is present, the test can confirm signs of anemia or bleeding in the colon, which can be a sign of early polyp growth. A Single Swipe Can Save Your Life
Talk to us and learn more about at-home colon cancer screening and on-site testing today. The post At-Home Colon Cancer Screening Tests: What You Need to Know appeared first on Gastro Center NJ. via Gastro Center NJ https://gastrocenternj.com/at-home-colon-cancer-screening-tests/ |
AuthorAt the Gastro Center of NJ, we prioritize your digestive health. Our highly trained professional gastroenterologists treat our patients with the most modern approaches and the most advanced medical technologies. We work towards accommodating the unique needs of every patient. We understand the value of health and happiness for your body and mind. Contact
Gastro Center NJ 59 Main St Suite 1, West Orange, NJ 07052, USA Phone: +1-862-520-1696 Email: [email protected] Website: https://gastrocenternj.com/ FIND US ONLINE 500px Bitly Box Diigo DropBox Evernote Postach.io Instapaper NewsBlur Nimbus OneDrive OneNote Quip Todoist Todledo Trello Tumblr Weebly Wordpress Blogger Google Drive Youtube aboutme.google Recommended Links About.me Alternion Brandyourself.com Followus.com Gravatar Behance.net Linkkle Ello.co Carrd.co Scoop.it Zumvu iLink ArchivesNo Archives Categories |


 RSS Feed
RSS Feed
